When epilepsy isn't epilepsy
Epilepsy vs Non-Epileptic Seizures and Psychogenic Non-Epileptic Attacks
Stress is a well established seizure trigger, a fact that is incontrovertible.
Stress has the ability to provoke seizures through various mechanisms, such as hormonal changes, increased neuronal excitability, sleep disruption, emotional responses, biochemical alterations, autonomic nervous system activation, and immune system activation.
These factors can potentially induce seizures in ANY individual subjected to sufficient stress (as they disrupt the brain's normal balance), but most ‘normal people’ have a high threshold. It goes without saying of course that individuals with a history of epilepsy or any kind of acquired brain injury are especially vulnerable. Their threshold for seizures is likely to be significantly lower due to pre-existing neurological issues. I’m stating the obvious, but it’s important for context.
Why is this important?
When managing a condition like brain tumour related epilepsy or forms of epilepsy that are generally not of a spontaneous nature, it is crucial to be able to distinguish between epileptic seizures and stress-related attacks that might mimic seizures, but are actually Psychogenic Non-Epileptic Attacks (PNEAs) or other types of non-epileptic seizure disorders.
Many people fail to realise that there are many different types of epilepsy. As a matter of fact, there are over 100 different types of epilepsy when considering the various combinations of seizure types, origins, and specific epilepsy syndromes.
PNEAs can be categorised under the umbrella of ‘reflex epilepsy’, a type of epilepsy where seizures are triggered by specific stimuli or activities.
Why should we care so much about reflex epilepsy?
It has become apparent to me that reflex epilepsy is a form of epilepsy that is under-recognised, under-appreciated, and possibly under-diagnosed.
I believe I am well-positioned to comment, as I live with reflex epilepsy and have gained considerable knowledge about it. I self-diagnosed after identifying all my triggers, noticing patterns, and realising that the episodes I was experiencing were not spontaneous. Along the way I was offered no support or guidance, and was made to feel that some of these symptoms were just ‘in my head’ (in the figurative sense), so I hope writing this helps others.
I suspect many more people also have this type of epilepsy, but they are unaware. I also feel as though neurologists often overlook the importance of recognising reflex epilepsy and differentiating it from other forms of the condition. I had to discover all this on my own. Of course there will be some overlap with epilepsy in general, to varying degrees among individuals.
Although controversial, my case closely mirrors the form of epilepsy mentioned in this example, not by cause, but how it is triggered. This sub-type of reflex epilepsy is termed ‘Eating reflex epilepsy’, and is the primary reason I was compelled to go beyond a traditional ketogenic diet by adopting an ‘oligoantigenic ketogenic diet’. This is because I was developing an allergic-like reaction to certain foods, triggering seizures along with more subtle symptoms.
I don’t actually think this ‘Eating Reflex Epilepsy’ phenomena is that uncommon, it’s just that few people mention it. We need to go beyond looking at blood glucose and/or blood ketones when treating epilepsy with diet and we need to carefully observe reactions to different foods, even if they are classed as ‘ketogenic’.
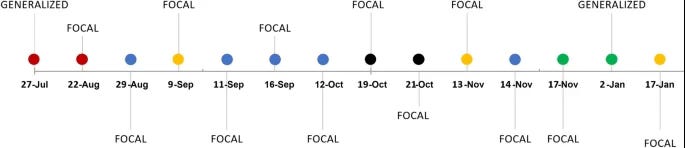
We all have different reactions, one way of testing is to follow an oligoantigenic diet to remove all known common allergens (eg. nuts, dairy, egg whites, shellfish, gluten soy) and assess the response of that before doing anything else. These hypoallergenic diets have a long, established history in treating epilepsy and migraine disorders as evidenced by this review, examples from individual case studies and studies positing a catalytic role for inflammatory processes in the pathophysiology of epilepsy.
While reflex epilepsy is (apparently) relatively rare, it can tell us a huge amount about individual variables in epilepsy disorders, why they happen, mechanisms between the underlying aetiology, physiological systems involved, brain connections, regions affected and how we can possibly prevent them from occurring.
Even the rarest forms of reflex epilepsy, for example this case study involving the limbic system activated, resulting in seizures triggered by towels, can provide valuable insights.
In my case, I can experience a migraine-like aura upon encountering known stimuli triggering my seizures. I’m not sure whether the migraines are concurrent or act as a catalyst to seizures, but because they are now so infrequent I don’t give this as much thought as I used to. What I do know is that, if I were to suffer a recurrence of disease, it is likely that these symptoms would worsen, and I have contingency plans for this.
Symptoms can tell you a lot about disease and there is a lot to be said for feeling good. If you’re trying all these therapies and strict diets to treat a serious disease and you feel like crap, that's not ideal. My first port of call if I were to suffer a recurrence would be to control the symptoms as best I could with treatments that have a dual function (management of symptoms and as cancer treatment).
Due to the location of residual disease that is at present no longer visible, I predict a recurrence would involve a grand mal seizure, followed by episodic migraines and nausea. I would re-introduce epilim (sodium valproate) to manage the seizures and for it’s anti cancer benefits, take different forms of magnesium more regularly (L-Threonate, Glycinate, Citrate), increase melatonin, begin taking a CGRP antagonist for the migraines (find out why here), and I would put myself on an anti-emetic drug that has shown anti cancer benefits for glioma. I would also occasionally chew on a gum containing xylitol, like Kaigum, to activate the vagus nerve and additional reasons I won’t go into here. Equally important, from a quality of life aspect, if you feel as though you are doing all the right things and you maintain a parasympathetic state, you can reduce the likelihood of PNEAs.
What are Psychogenic Non-Epileptic Attacks?
Firstly, we must establish that although they can be very serious, psychogenic non epileptic seizures (PNEAs), are not epileptic in nature. They arise not from the abnormal electrical discharges in the brain that characterise epilepsy, but rather from psychological factors.
The last thing we want to be told is ‘it’s all in your head’, because that simply isn’t true in most instances. What I’m referring to is more a scenario where an individual is prone to having seizures, may experience an ‘aura’ as a warning a seizure is due to occur and they have a choice…
…They can either focus on the aura and panic, - which is an understandable reaction, but makes things worse - or they could try damage control by
Keep reading with a 7-day free trial
Subscribe to Andrew’s Substack to keep reading this post and get 7 days of free access to the full post archives.




